Here’s an example: Jason is a single man in his early 30s and has always been insured by his employer.
A month ago he was told he would no longer have health insurance coverage through his job. He feels overwhelmed navigating the insurance world on his own and is unsure of his next steps.
He’s looked at COBRA coverage, but the premium payments are too expensive without the help of his employer, and he wants to find a plan that’s best for his needs.
You may qualify for a special enrollment period.
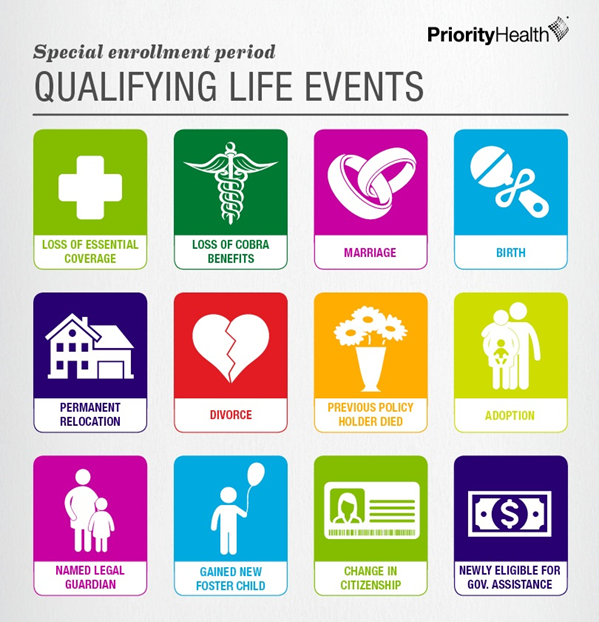
Although the open enrollment period for health insurance is over, losing job-based health insurance is a qualifying life event (QLE), which means Jason qualifies for a special enrollment period (SEP). A special enrollment period allows you and your family to enroll in or change your health plan outside of the open enrollment period.
Losing employer-sponsored health insurance isn’t the only qualifying life event. Other QLEs include moving to a new state, getting married or aging out of your parents’ health plan. If you’ve had a life change, you may be able to enroll in a new health plan through a health insurance carrier or the federal health insurance marketplace. Don’t forget to check if you’re eligible for a subsidy—you could reduce the cost of your monthly premium and out-of-pocket expenses if you qualify.
You qualify for an SEP, now what?
The sooner you take action, the better. Don’t let time escape you after you’ve lost coverage— you’re only allowed 60 days following a QLE to make changes to or enroll in a new health plan. Once you’re enrolled, your new coverage typically takes effect as quickly as the first day of the following month from the date you lost coverage.
Don’t go uninsured.
If you opt to forgo health insurance for all or part of the year, you won’t be able to enroll in an insurance plan until the next open enrollment period. This means you won’t be covered in the event of an unexpected illness or injury, which could be financially devastating as the average cost of a 3-day hospital stay is approximately $30,000, according to Healthcare.gov.
If you have questions about your coverage options, consult with a licensed insurance agent or request information from a trusted insurance provider. These resources are available to make sure you get a plan that’s right for you and your family. Whether you opt in to COBRA coverage or enroll in a plan during a special enrollment period, the most important thing is that you and your family are covered. To learn more about Priority Health’s plans, visit our website.