By Ann Donnelly, BSN, RN, MA
Nearly 14,100 women will be diagnosed with cervical cancer in 2022, and an estimated 4,280 women will die from cervical cancer this year. But if detected early enough, it is one of the most treatable forms of the disease.
Cervical cancer is preventable and treatable, thanks to screenings and vaccinations. If found in the early stages when cancer has not spread outside the cervix or uterus, the five year survival rate for cervical cancer is about 92 percent.
Get your screenings regularly.
One of the best ways to reduce your risk of cervical cancer is to get a Pap test, or Pap smear, and human papillomavirus (HPV) test done by your doctor. The human papillomavirus (HPV) is the most common sexually transmitted disease (STD) that plays a role in causing cervical cancer.
These tests find precancerous cells before they turn into invasive cancer, improving the chances of successful treatment.
According to the American Cancer Society:
- All women should begin cervical cancer screening at age 25, however, some health plans will cover screenings as early as 21 years old. Check with your health plan for screening and coverage options.
- Women aged 25 to 65 should have a HPV test every five years.
- Women aged 25 to 65 should have a Pap test just once every three years, or have a combined Pap and HPV test every five years.
- Women aged 65 and older who have had regular screenings for 10 years with normal results do not need to be screened for cervical cancer. Those diagnosed with cervical pre-cancer should continue to be screened.
- Women who have had a total hysterectomy and no history of cervical cancer or pre-cancer do not need to be screened.
- Women who have had the HPV vaccine should follow the screening recommendations for their age group.
- Women at high risk for cervical cancer – including those with HIV infections, organ transplant recipients or those exposed to DES, a synthetic estrogen, while in utero – may need to be screened more often and should consult their doctor.
Consider the HPV vaccine for cervical cancer prevention.
In most cases, the HPV virus causes no symptoms or health problems and can go away on its own. But, for about 10 percent of women, persistent HPV infections on their cervix put them at greater risk for developing cervical cancer.
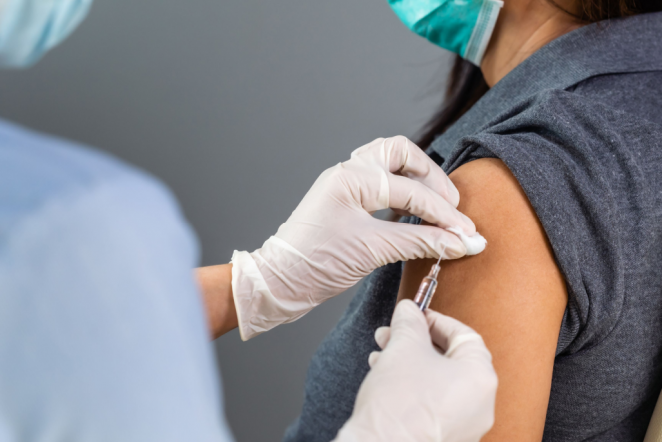
The HPV vaccine can protect against four HPV types, including two high-risk strains that cause most cervical cancers. The Centers for Disease Control and Prevention recommend this vaccination, which must be given in two to three doses, for teens and young adults of all genders aged 11 to 26.
The vaccine should be given before an HPV infection occurs, and ideally, before they become sexually active. While your teen may not be sexually active, it’
s important for parents to consider the vaccine for cancer prevention well into adulthood. Those aged 26 and older are not recommended to get the HPV vaccine as it is less effective for cancer prevention.
Stay in charge of your own wellbeing.
In addition to regular screenings and vaccinations, maintaining a healthy lifestyle can go a long way towards preventing cervical cancer. Under the Affordable Care Act, the HPV vaccine should be 100% covered. Your health plan also likely covers cervical cancer screening as part of preventive health care, meaning you can receive these services at no additional cost.
Keep in mind that if your screening detects a potential health problem and the doctor requests further testing, you will likely need to split a portion of the cost for these additional tests with your health plan.
Know your risk factors and check with your doctor on how to lower your chances of developing cervical cancer. Get ahead of certain health problems and risks with preventive care.

About the author: Ann Donnelly, BSN, RN, MA, is vice president, care management and operations at Priority Health. In this role she leads the care management and operations departments, managing teams who problem solves solutions to control unnecessary costs and improve the health of Priority Health’s members through personalized care management. She has been instrumental in launching and improving programs including diabetes prevention, medication therapy and complex care management.